Foot Fungus Misdiagnosis As Bacterial Infection Causing Cellulitis, Foot Pain, Rash, Fever
Created: Sept 6, 2020by Salvatore Crapanzano, C.C.Ir., B.A.Sc., M.A.Sc.
As someone who suffered a serious long-term Candida infection for more than 10 years, many years ago, I was not expecting to urgently require antibiotic usage for a foot infection by the bacterium Staph.
In fact, the last time I took some antibiotics for a short course was in 2001, over 17 years ago when I lived in Vancouver and was trying to decipher the effects of mold exposure in my apartment (before I became a natural health practitioner).
I knew at the beginning of 2018, that I had a mild fungal infection in my body.
My crotch had slightly red lines like a V on both sides, and it looked vaguely like the toilet bowel red if it was not cleaned soon enough.
The fungus was not from eating cheese for one of my meals per day on a regular basis. (Cheese has fungus in it.)
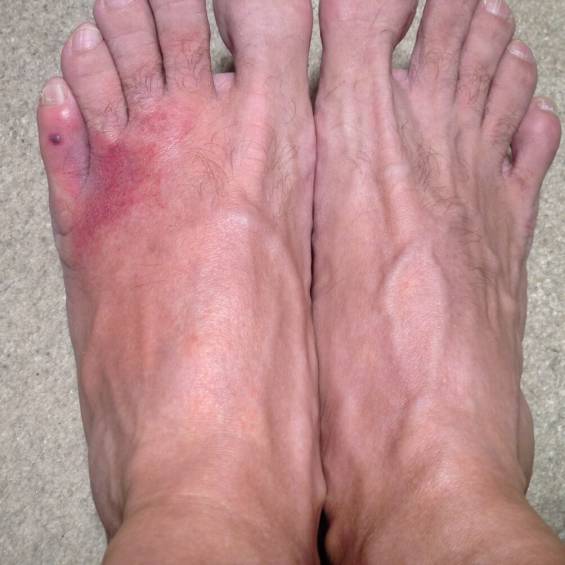
Inflammation, redness and heat in the left area of my foot. Also a red ash along the pinky toe.
How It All Started: Pain in the Foot Leading to a Diagnosis of Cellulitis (Skin Infection)
I went out to grocery shopping on Saturday October 13, 2018. I would estimate I was on my feet for about 4 hours, and came back with much pain in the left foot.
With my feet out of my shoes, I massaged the left foot, and I noticed that there was a large area of it around my pinky toe that was red, and painful. See the picture above.
The pain seemed to come from the left pinky in my left foot. And there was an area all over and behind my toes that was painful to touch.
I erroneously believed that during cooler fall weather my foot had shrunk a little and had rubbed against the shoe too much, and then irritated my left pinky toe. Running shoes don't fit perfectly all the time of course.
And I was rather confused because the toe nail did not hurt.
So, I attributed this sudden foot pain to this pair of fairly new running shoes, purchased only 4 months previously.
I thought these shoes were great for the summer (purchased end of June 2018), because the feet expand during summer, and when October and colder weather came to the West Coast the extra space for the feet caused them to hit the shoe.
I could also see there was some wear in the inner lining where the pinky rested.
I was concerned and massaged the foot while I was in bed.
I kept thinking the problem was my left pinky toe.
You can see the picture below of my left foot's inflammation even after I started taking antibiotics.
Later (see below) I learned from physician #2 that after I was properly diagnosed from physician #3 (with a fungal infection which caused me a very serious recurring bacterial infection), that only 1 out of 20 people who have cellulitis get pain, and sometimes extreme pain.
I will detail chronologically how this occurred more fully below.
Proper Diagnosis of a Root Cause Fungal Infection
Doctors are not going to rush to give you antibiotics when the diagnosis could not be cellulitis. As this medical document for the province in Quebec, Canada states, it requires a differential diagnosis because other diagnosis could mimic it. Drug Antibiotics Cellulitis in Adults.
I will also relate another interesting story brought forth by physician #2 who diagnosed me with the recurring cellulitis.
I can relate to this important story because in my University years, I had food poisoning and went back to the Emergency department of the local hospital 3 times before I got a proper diagnosis. I was finally told then that I had food poisoning and that I should have been put on antibiotics.
This primary care physician #2 who diagnosed me with the recurring cellulitis (once the first round of antibiotics failed) had once worked in an Emergency department and cared for a woman who also came back 3 times until she finally got diagnosed with Cellulitis. She had reddened skin on her leg.
She had pain so she went back. Initially they thought she had arthritis.
He made a proper diagnosis, and she was given antibiotics for this infection pronto.
He mentioned that if you have cellulitis, you must get on Antibiotics within 5-7 days of initially showing signs because this type of infection can turn into Necrotizing Fasciitis, or flesh-eating disease!
My Initial Visit with Physician Cellulitis Diagnosis #1 + Antibiotic: Clindamycin:
October 16, 2018, I finally decided to walk in, and see a physician. Three days after the pain started and did not end.
My diagnosis was cellulitis, a skin infection. I was given a prescription for a 10 day course of Clindamycin 300mg.
Clindamycin is one of the drugs of choice for skin and soft-tissue infections (1).
When I discussed the cause of this, the physician indicated it was not the shoe. She did examine my toes very casually.
You can see the picture of my skin being eaten away from the left pinky toe just below.
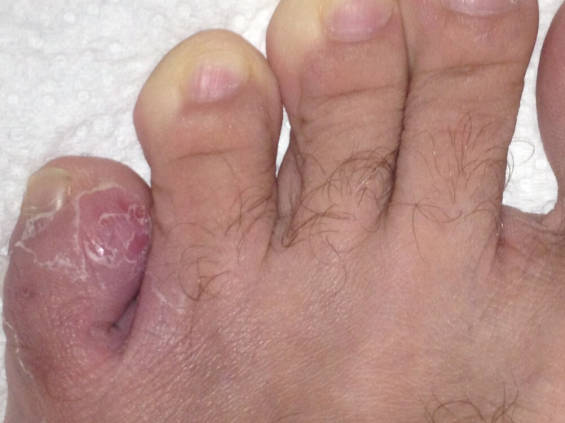
Being between the two left most toes of the left foot, the skin was macerated as the third doctor declared. As he explained it, like when you take long, long baths. Or shriveled skin falling off as I put it.
In actuality the skin was being eaten by a fungus (Diagnosis #3). The root diagnosis was a fungal infection. Probably the fungus that causes athletes foot.
Why the antibiotics for the cellulitis.
Quoting the Canadian Journal of Infectious Diseases paper cited above:
Like cloxacillin and the cephalosporins, clindamycin possesses activity against Staphylococcus aureus.
My infection was diagnosed as Staphylococcus aureus cellulitis :
That is invasive Staphylococcus Aureus. This is just a probable diagnosis based on visual inspection and history. There is no culture or skin biopsy test given to me.
According to the above publication: Experts recommend Clindamycin be used in conjunction with other antibiotics such as penicillin for severe group A infections such as necrotizing fasciitis.
Physician #1 mentioned that my foot infection cellulitis, could turn in Sepsis (Septicemia). Sepsis means the infection has entered the bloodstream.
Sepsis (Septicemia) is a very serious infection.
And again, In any kind of cellulitis, there is a chance the infection will turn into Necrotizing fasciitis according to the second physician I saw.
Therefore he re commended treatment with antibiotics, and proper diagnosis be commenced within 5-7 days.
Bacterial cellulitis can become more serious as Necrotizing Fasciitis. Recommended to catch it early, stay on top of it, and get on antibiotics within 5 days of diagnosed.
Antibiotic Clindamycin side effect can cause Clostridium Difficile Colitis
Clindamycin is one of those antibiotics that can cause an infection and inflammation of the colon called Clostridium Difficile colitis.
When I found out that the side-effects were diarrhea from the pharmacist, I was not pleased. I later found out I could have been prescribed a different antibiotic without this side effect.
I was strongly recommended to take a probiotic because it could cause me diarrhea.
I was quite familiar with the medical repercussions of having a C. Difficile infection long-term.
I decided to continue eating a lot of high quality probiotic yogurt every day.
According to my hygienist some elderly people lose weight for several months and are then finally diagnosed with a C. Difficile infection because of bowel issues.
Diagnosis #2: Recurring Cellulitis
For my second physician visit, I had finished the first course of antibiotics, the Clindamycin, but after about 1 week I still felt sick again, with a minor fever.
The foot pain and redness had also come back, so physician visit #2 was warranted. This was very disappointing because the antibiotics are carefully taken away from food for effectiveness, and the second antibiotic was taken more frequently.
The second antibiotic was a penicillin, called Cloxacillin, 500mg. This was taken 4 X a day, instead of 3X a day originally with the Clindamycin. It was taken for 14 days.
Three weeks went by between the first diagnosis and the recurring diagnosis #2.
Proper Diagnosis #3 :Fungal Infection, Wound care
After diagnosis #2 of the recurring cellulitis in my left foot, I was asked to see a specialist in wound care.
The wound was in between the pinky toe and the 2nd toe, because there was an opening. That opening is probably how the Staph. Aureus penetrated the skin.
Luckily I got an appointment in 2 days time. The universe was in my favour.
Physician #3 had a specialty in dermatology.
He told me this was clearly a fungal infection, and prescribed a cream called Lamisil. The fungus had eaten my skin, and needed to be destroyed.
He also told me to use a small amount of vinegar diluted in water on the skin on my toe, and in between my toes before I put on the cream.
As the days went on after the Lamisil cream treatment, I saw the skin clearing up.
By and large, I'd like to say the second round of antibiotics needed was an inconvenience, because of the every 6 hour rule, and away from food.
Obviously that was needed because the cellulitis was raging and going to come back.
I was up at times after midnight taking the last round of this antibiotics, and at 5 or 6am taking my early morning dose.
My sleep rhythm was disturbed and it took some time to return.
The picture below shows some healing after about 3 days on the Lamisil anti-fungal cream and vinegar-water cleanup.
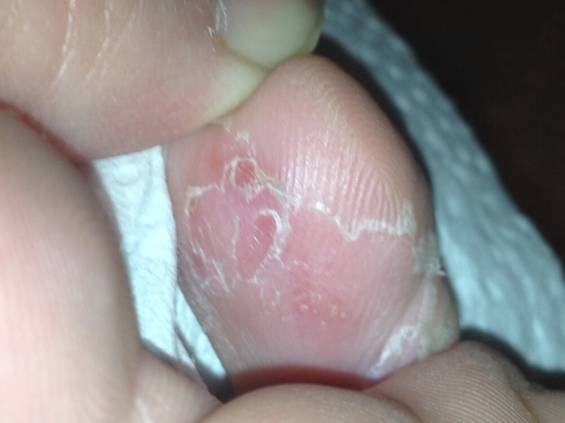
Need Help Healing?
Not felt right after cellulitis and antibiotic treatment? Your digestion affected? Need help cleaning up a C. Difficile infection?
How about a Candida infection?
Contact us today for help: